It began in earnest for me in January 2016. Four weeks after my Diagnosis of Stage 3c Invasive Lobular Breast Cancer which had spread to my Axillary nodes and to my Internal mammary nodes. I had never missed a Mammogram. I had no known Family History of Breast Cancer. I’d had my most recent Mammogram 6 months before my Diagnosis and it was reported as Clear. I really couldn’t get me head around how I now had “at least 5.5 cm Tumour” growing inside me when I’d been so diligent with my Screening Mammograms.
As I wrestled with a Diagnosis of Late Stage Cancer I began to question how after years of Clear Mammograms, I ended up with a Sizeable Tumour. How was it not Diagnosed Earlier? Was it Missed? How long had it been there? So many unanswered questions and very little Information about Lobular Breast Cancer.
I came across an article about an incredible woman called Nancy Cappello. Her Stage 3c Breast Cancer had also been missed following years of Clear Mammograms. The similarities between our late / missed Diagnoses were striking, although Nancy had Ductal Carcinoma (80% of Breast Cancers) and I had Lobular Carcinoma (15%)
Having read about Nancy and her grassroots Advocacy http://www.areyoudense.org, I was shocked to learn that 40% of us have Dense Breasts. It’s a Radiological finding and very visible on a Mammogram. It appears as white areas on Mammographic Images so it’s easy for a Radiologist to assess. The problem is however that Cancer also appears as white areas on Mammographic Images. Being that it’s so visible, why are women not told about it, after all, decades of research suggested Breast Density csn mask Cancer on a Mammogram. Was I Dense? How many women like me might have Dense Breasts and not know.
I wondered whether that could have been the reason why my Cancer was missed. I sought a second Surgical Opinion and this wonderful man disclosed to me “Your Breast Cancer is likely there 6 – 8 Years.”I decided to look at why had my Mammograms had let me down, why was the Cancer not found earlier? What needed to be done to alert Irish women about this. I founded http://www.beingdense.com Education and Awareness of Breast Density and associated risk factors.
WHITE on WHITE ‘Masking’ is one of the known Risk Factors for Women with high levels of Dense Breast Tissue
Because both Breast Cancer and Breast Density appear as WHITE Areas on a Mammogram – Breast Cancer can be easily missed on Screening Mammograms
Breast Cancers missed on Mammograms, sometimes found in between two Screenings, are referred to as Interval Cancers
Interval Cancers tend to be Larger at Diagnosis often with Nodal involvement
Clinical recall is NOT mandatory in Ireland for Women with Dense Breasts
Women have NOT been routinely Notified about their Personal Category of Breast Density
European Recommendations will now address this. “After careful consideration of the evidence, particularly the results of the Dutch DENSE trial, EUSOBI now recommends that women with extremely dense breast tissue are offered screening with breast MRI. In these women, breast MRI can reduce the mortality from breast cancer and is highly cost-effective”
The European Society of Breast Imaging has issued these recommendations
https://link.springer.com/article/10.1007/s00330-022-08617-6
It is so important to ask about YOUR personal Category of Breast Density A B C or D
C and D are considered to be Dense Breasts
D being Extremely Dense
To Request Your Personal Category of Breast Density you can download our Request Form, add your details and submit https://acrobat.adobe.com/link/review?uri=urn:aaid:scds:US:a8da5015-1c6b-4c61-ae1e-7fc29497d171 “EUSOBI thus calls on all providers of mammography screening to share density information with the women being screened.”
More information on Beingdense.com
http://www.Beingdense.com
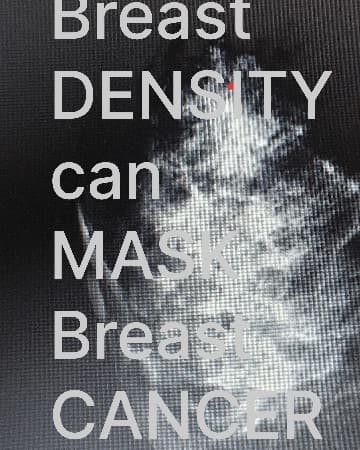

“An Interval Cancer”
Thr excerpt below from #EUSOBI Recommendations clearly indicate the significance of a Notification Protocol around Informing Women about their Personal Category of Mammographic Breast Density as seen on their Screening Mammogram

“These women are, therefore, underserved with current mammographic screening programs. The results of recent studies reporting on contrast-enhanced breast MRI as a screening method in women with extremely dense breasts provide compelling evidence that this approach can enable an important reduction in breast cancer mortality for these women and is cost-effective. Because there is now a valid option to improve breast cancer screening, the European Society of Breast Imaging (EUSOBI) recommends that women should be informed about their breast density. EUSOBI thus calls on all providers of mammography screening to share density information with the women being screened. In light of the available evidence, in women aged 50 to 70 years with extremely dense breasts, the EUSOBI now recommends offering screening breast MRI every 2 to 4 years. The EUSOBI acknowledges that it may currently not be possible to offer breast MRI immediately and everywhere and underscores that quality assurance procedures need to be established, but urges radiological societies and policymakers to act on this now. Since the wishes and values of individual women differ, in screening the principles of shared decision-making should be embraced. In particular, women should be counselled on the benefits and risks of mammography and MRI-based screening, so that they are capable of making an informed choice about their preferred screening method.“

